Summary
Healthcare organizations do not suffer from a lack of outreach. They suffer from a lack of relevant, timely, coordinated engagement. Member data is fragmented across claims, pharmacy, clinical, demographic, social, and engagement systems. Outreach is often built around static segments, disconnected tools, and one-size-fits-most campaigns. The result is a familiar pattern: high administrative effort, low program uptake, wasted spend, avoidable care gaps, and member experiences that feel impersonal.
RadiantGraph’s Intelligent Personalization is designed to solve that problem using AI and omnichannel outreach, including AI Voice Agents. Built specifically for healthcare, RadiantGraph is an intelligence and engagement platform that unifies fragmented member data, identifies who needs what support and when, and orchestrates prioritized and personalized outreach across multiple channels to drive measurable outcomes. Rather than forcing organizations to replace existing systems, RadiantGraph sits between member data and engagement tools as a composable intelligence layer.
RadiantGraph operates across three integrated phases to turn legacy reactive outreach into proactive, personalized member engagement at scale:
Activate: Unifies and enriches disconnected data and surfaces AI-driven signals
Platform Offerings: Health Data Engine and Population Explorer
Personalize: Identifies the right people, messages, and resource allocation.
Platform Offerings: Smart Cohorts and Smart Spend
Engage: Orchestrates HIPAA-compliant, segment-tailored outreach and optimizes channel distribution from AI-powered insights.
Platform Offerings: Journey Builder, Content Co-Creator, and AI Voice Studio
The business case is not theoretical. Across RadiantGraph customers, results include significant improvements in outreach, enrollment, registrations, hours saved, and human efficiency generating reductions in OPEX, outbound calls, and outreach time. These proofpoints demonstrate Intelligent Personalization is not just another “engagement” point solution, but as a way to improve activation, close care gaps earlier, reduce waste, and use limited operational and clinical capacity more effectively.
Who Is RadiantGraph
RadiantGraph was founded on a simple observation: healthcare organizations already have the data they need for outreach that drives meaningful outcomes for members, but lack the ability to turn it into timely, coordinated action. The company launched publicly in October 2023 after raising a $5 million seed round (True Ventures and XYZ Ventures), and announced an $11 million Series A in October 2024. Throughout its history, RadiantGraph has focused on continuous expansion of platform capabilities, the most recent of which is AI Voice Studio, released in June 2025. Also in June, Databricks awarded RadiantGraph a $1 million grand prize in its startup challenge, backing further platform expansion.
The company is led by founder and CEO Anmol Madan, PhD, whose background includes senior AI leadership roles at Teladoc and Livongo, and co-founding Ginger. Anmol’s experience is central to his founding thesis: after years building AI products across healthcare, Madan concluded that consumer engagement is a core bottleneck in healthcare economics and outcomes. In his words, healthcare entities, plans, and employers are not seeing adequate return on their engagement investments, and consumers are not fully benefiting from digital health innovation.
RadiantGraph was built for realities of healthcare - fragmented data, regulatory complexity, and operational constraints – and is not a generic customer engagement platform shoehorned into healthcare ecosystems. It enables organizations to move beyond conversion and drive meaningful next-best actions like closing care gaps, completing HRAs, enrolling in programs, and ensuring follow-up care.
Introduction and Problem Statement
Healthcare interactions are still too often reactive, generic, and operationally expensive. Health plans and other healthcare entities invest heavily in outreach programs, experience teams, call-center operations, digital tools, and care-management workflows, yet many members still miss preventive screenings, delay follow-up care, fail to complete HRAs, or never enroll in programs that could improve their outcomes. The issue is not the absence of programs - it is the inability to consistently translate available data into the right action for the right person at the right time.
That gap is becoming more costly as member expectations rise. Consumers increasingly expect healthcare interactions to feel as relevant and personalized as the best experiences they receive in other industries. When outreach feels generic, mistimed, or disconnected from real need, members ignore it, delay care, and lose trust. For healthcare entities, these engagement failures translate into lower quality performance, weaker retention, higher cost to serve, lower program adoption, and underperformance from existing technology and outreach investments.
Healthcare organizations therefore face a strategic challenge, not simply a communications challenge: how to turn fragmented data into proactive, coordinated engagement that improves both member experience and business performance. RadiantGraph’s Intelligent Personalization is designed to address that challenge directly.
Why the Problem Exists
The problem exists because healthcare engagement is constrained by both data architecture and operating model. Most organizations are not starting from a blank slate; they are operating within a complex environment of siloed data, fragmented workflows, limited capacity, and rising performance expectations.
First, data is fragmented. Claims, pharmacy, clinical, demographic, social determinants, contact data, and historical engagement signals often live in different systems and formats. RadiantGraph calls the hidden cost of this fragmentation the “data tax.” Without unification, teams rely on incomplete records, delayed reporting, and manual audience construction. The result is slow execution and weak personalization, or the pain which comes from multi-year rebuilds typical of legacy fixes.
Second, healthcare organizations commonly operate with static stratification and broad campaigns. Intuition and “internal momentum” still drives many campaigns because data is disparate, lead times are long, and content teams must work inside rigid compliance guardrails. In practice, that means HCEs tend to over-contact some, under-support others, and miss the nuances that influence action: readiness, language, confusion, access barriers, preferred channels, and timing.
Third, the economics of outreach are unforgiving. Human care teams, clinicians, and call-center agents are limited resources. Many high-value interventions require prioritization, not just volume. The reality is the scarce resource is often not just the budget dollars, but care-team capacity and intervention availability. What’s needed is the ability to rank-order people by likelihood to benefit in order preserve outcomes and reduce unnecessary workload.
Fourth, the broader market environment exponentially increases the cost of getting engagement wrong. Policy changes such as reimbursement levels, Medicaid qualification requirements, and ratings components materially affect plan performance and member retention. Furthermore, the spotlight is directly shining on plans – KFF reports that health-care affordability remains one of the public’s top economic worries (kff.org). In short, the risks of not having better member identification, education, and guided action at scale are higher than ever.
Introducing Intelligent Personalization
Intelligent Personalization is RadiantGraph’s healthcare-specific approach to turning disconnected data into proactive, personalized engagement. It enables healthcare organizations to identify who needs what support, when they need it, and how they are most likely to respond, then act on that intelligence through coordinated outreach across channels. Put simply, Intelligent Personalization turns fragmented healthcare data into the right message for the right member at the right time through the right channel.
What differentiates the concept is that it is not just a campaign tool, data warehouse, or communications channel. Instead, Intelligent Personalization is an action layer sitting between data systems and engagement systems. It plugs into warehouse and EHR environments such as AWS, Azure, Databricks, Snowflake, Redshift, Google Cloud Platform (GCP), and Epic and connects with engagement tools such as Braze, Salesforce Marketing Cloud, Pega, Iterable, Twilio, Adobe, and Genesys. RadiantGraph believes in augmentation rather than wholesale replacement of existing investments. However, if desired, RadiantGraph can also be the last-mile engagement tool, especially with AI Voice Studio.
RadiantGraph organizes the platform around three phases:
Activate: RadiantGraph authenticates access, unifies fragmented data, resolves identity and formatting problems, enriches profiles with missing information and third-party context, and makes the data usable for visualization and AI-driven engagement.
Personalize: RadiantGraph moves from data to decisions dynamically grouping members based on clinical, claims, SDoH, behavioral, and engagement signals that helps organizations focus resources where they are most likely to generate return.
Engage: RadiantGraph orchestrates HIPAA-compliant, multi-step, omnichannel journeys across AI voice, email, SMS, direct mail, and more. The point is not to send more messages; it is to coordinate timing, content, channel, and escalation logic around consumer readiness and operational goals.
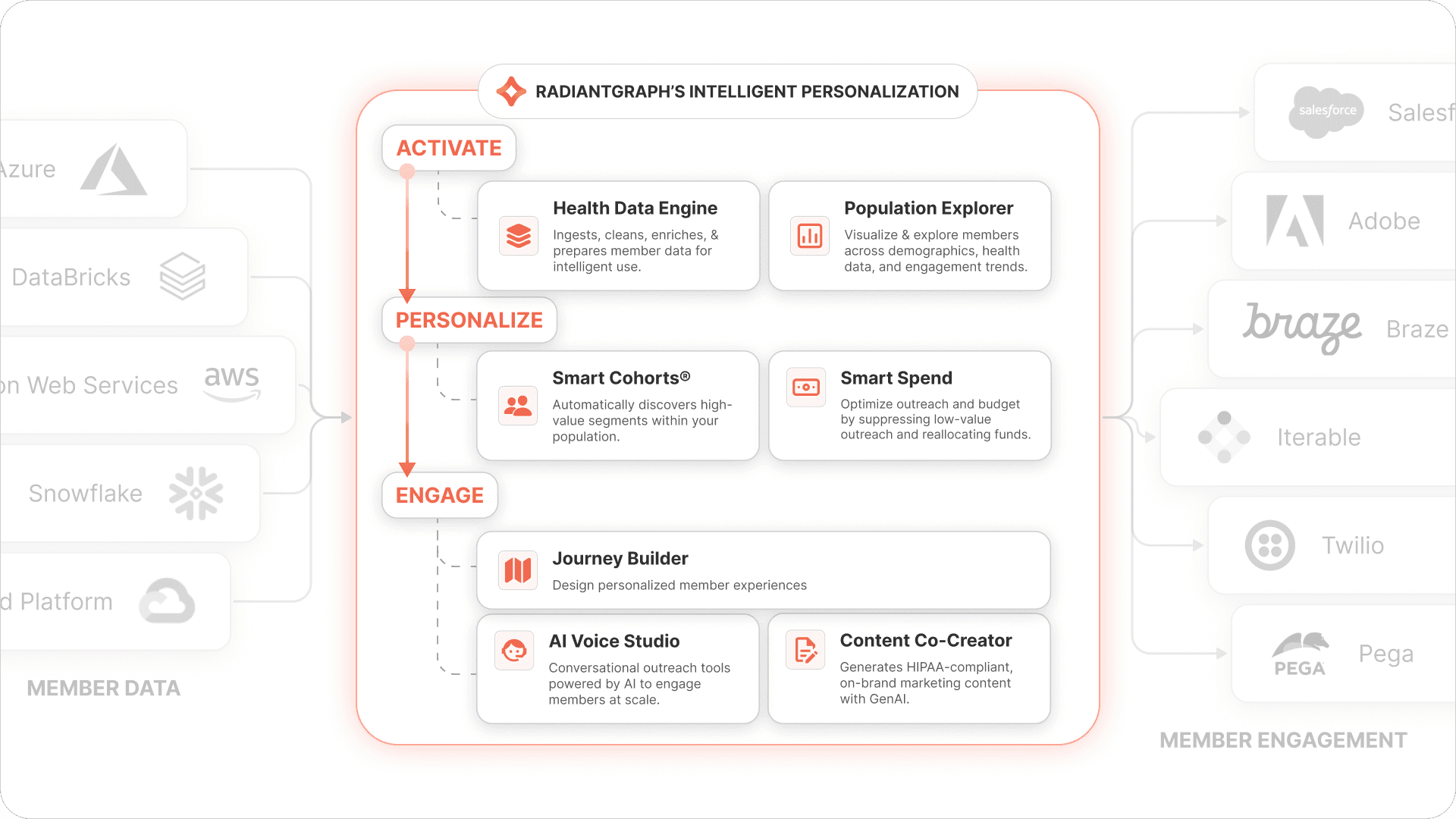
How Does Intelligent Personalization Work?
The platform narrative is straightforward: Activate → Personalize → Engage. In practice, that model translates into the following operating flow.
Data is authenticated, unified, transformed, and enriched: RadiantGraph begins with secure, HIPAA-aligned access to relevant data. The Health Data Engine unifies claims, pharmacy and clinical data, demographics, SDoH, contact information, and engagement signals. It also addresses common data issues such as ID resolution, deduplication, format standardization, and feature engineering. AI-based engagement can be live in weeks rather than the quarters or years often associated with traditional data-platform projects.
The system identifies patterns and opportunity areas: Population Explorer helps teams move from a unified data asset to decision-ready insight. Users can explore populations and sub-groups, compare trends, identify emerging risks or access constraints, and form hypotheses that then inform downstream segmentation and campaign design. The result is a more evidence-based starting point for outreach strategy.
RadiantGraph’s counter to static segmentation is Smart Cohorts: Consumers are grouped dynamically based on need, readiness, and likely response. Rather than locking people into broad demographic buckets, it dynamically assigns them to behavior- and context-driven groups using claims, clinical, SDoH, behavioral, and engagement signals.
Example cohorts include parents with young children, behavioral-health-at-risk members, access-constrained members, PCP-detached adults, low-awareness benefit populations, and chronic-condition-management patients. The same clinical program can look very different to different members, so cohorting informs not only who is targeted, but how.
Resources are prioritized where they can have the most impact: Smart Spend rank-orders members by likely responsiveness, clinical relevance, or expected return on engagement investment. In outreach-heavy use cases, that can mean de-prioritizing low-yield members from costly campaigns. In care-management contexts, it can mean directing scarce clinician or agent capacity to the members who are most likely to benefit from higher-touch intervention. This is how Intelligent Personalization moves from personalization as messaging to personalization as resource allocation.
Content is tailored to cohort context while staying safe and compliant: Content Co-Creator allows nontechnical teams to move from insight to message variants faster, with multilingual support, cohort-specific tailoring, healthcare communication standards, and human oversight. RadiantGraph’s AI does not replace marketers, clinicians, or consumer-experience teams; instead, it automates drafting, adaptation, and iteration while humans retain responsibility for strategy, judgment, and approval.
Journeys are orchestrated across channels: Journey Builder turns content decisions into omnichannel execution. It coordinates AI voice, email, SMS, direct mail, and other channels into multi-step journeys with branching, timing rules, and escalation paths. For example: a member may receive priming via mail or SMS, followed by AI voice outreach, then reminders or handoff options based on response. This allows engagement to adapt over time rather than forcing every person through the same sequence.
AI Voice Studio extends personalization into conversations: For use cases where phone outreach matters, AI Voice Studio allows healthcare organizations to launch healthcare-specific voice experiences with compliant guardrails, scenario testing, QA, escalation handling, and feedback loops. Member context informs each interaction, validated flows guide conversations, and performance data feeds continuous optimization. AI Voice Studio is a scalable way to handle routine outreach while preserving human teams for more complex or sensitive situations.
Performance data feeds continuous improvement: Intelligent Personalization is a learning system. As engagement data accumulates, audiences can update, campaigns can improve, and teams can refine targeting, timing, content, and channel mix over time. This matters because healthcare engagement is rarely solved by a single campaign. It improves when data, targeting, content, and channel strategy are refined continuously.
How Intelligent Personalization Creates ROI for Customers
RadiantGraph’s value proposition is straightforward: Intelligent Personalization helps healthcare organizations improve engagement outcomes while reducing the cost and operational burden required to achieve them.
Better member activation and outcomes – By identifying people earlier, reducing friction, and personalizing journeys, Intelligent Personalization helps organizations move members into screenings, visits, assessments, onboarding actions, and clinical programs sooner. For customers this means faster gap closure, improved registration, and more timely care activation.
More efficient use of outreach and care-team capacity – RadiantGraph is about efficiency: fewer wasted touches, better prioritization of members needing high-touch resources, and automation of lower-complexity interactions. This is especially valuable for HCEs with limited care-management or call-center capacity. Smart Spend and AI Voice Studio together support a model in which humans focus where empathy, judgment, or clinical escalation matter most.
Lower wasted spend – Because Intelligent Personalization helps rank members by propensity and fit, plans can trim unnecessary outreach without sacrificing outcomes. This is not just a messaging improvement; it is a budget discipline tool. One example is preserving registrations while reducing human outreach volume lowering spend per conversation.
Faster time to value – RadiantGraph prioritizes creating value quickly. The Health Data Engine can be producing results in roughly a month versus multi-year legacy project timelines, and AI Voice Studio can go from pilot to production equally quick. Both deployments then move to continuous optimization. For buyers wary of large transformation programs, that faster time to impact is a significant part of the value proposition.
Better member experience and trust – When members receive outreach that reflects their circumstances, preferred channels, and likely barriers, communications feel less like generic marketing and more like support. We believe in easier paths with clear next steps and more empathetic interactions. This approach supports quality, retention, NPS, and plan differentiation, especially in onboarding, navigation, and preventive-care use cases.
RadiantGraph’s case studies and deployment examples demonstrate ROI at two levels: immediate operational efficiency and strategic business performance.
Immediate Operational Efficiency
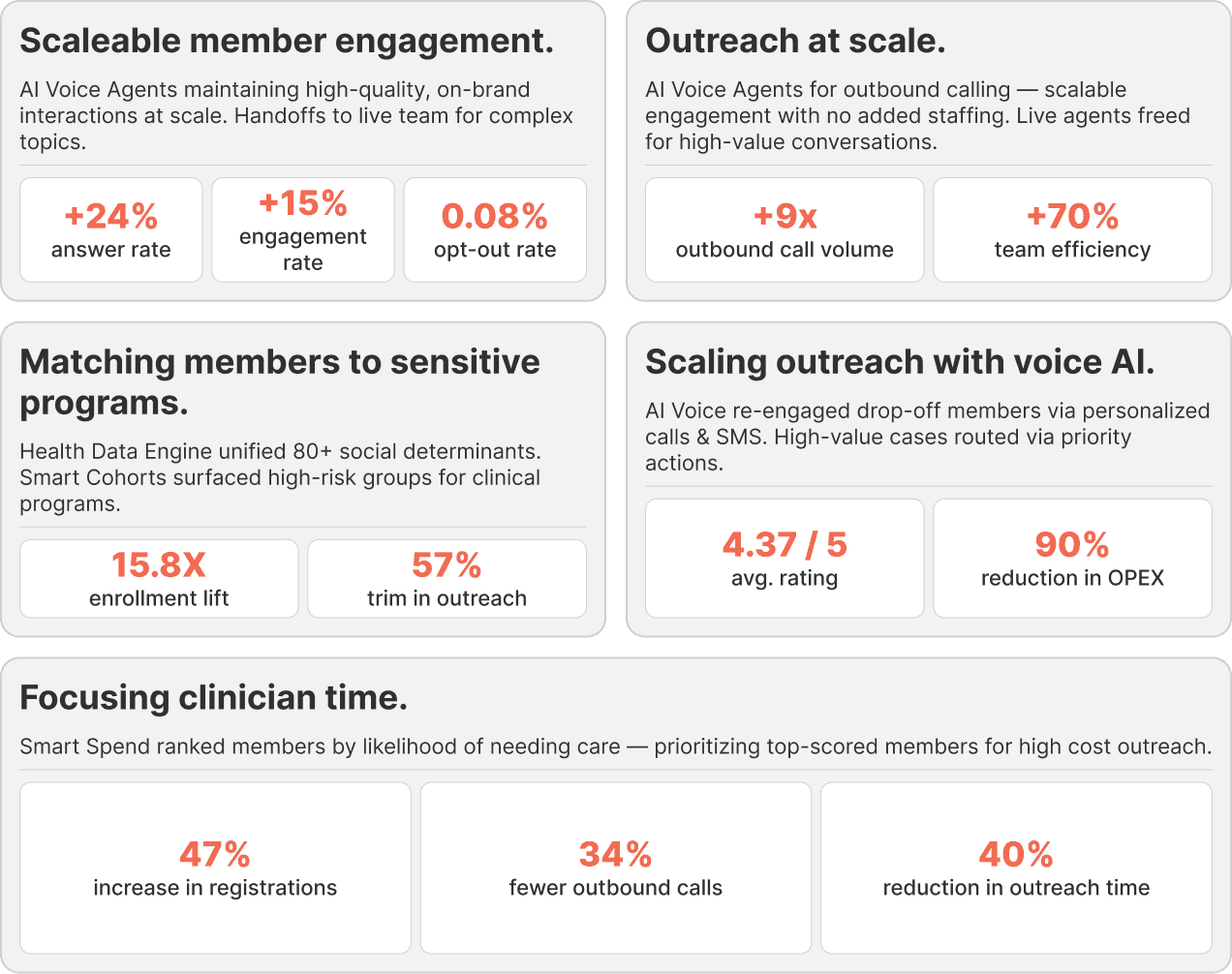
RadiantGraph also frames ROI at the strategic level. The major problems we address are often $50M+ business pain points including STARs improvements, redetermination-driven membership loss, and age-in churn. But the list does not stop there, strategic payoff also comes from lower MLR, improved retention, stronger member experience, better leverage of existing technology investments, and faster response to business priorities. Put simply: Intelligent Personalization is meant to influence high-value business outcomes, not just tactical metrics.
From a finance and operations perspective, the ROI logic comes from many levers:
Higher conversion on valuable actions such as screenings, HRA completion, onboarding, and program enrollment
Lower cost per completed action through better targeting and channel (including AI voice) mix
Lower operating cost via automation
Reduced MLR and improved downstream clinical and quality through earlier action and better adherence.
Higher NPS because of more relevant, timely, and coordinated member interactions that reduce frustration, improve trust, and make the overall experience feel more supportive and personalized.
The ability to leverage existing tech and clinical investments generating more value from the systems, programs, and teams customers already have in place, rather than adding yet another disconnected point solution.
Better ratings and scores due to improved member activation, stronger engagement in preventive and quality-related programs, and more consistent completion of the actions that influence performance measures.
Rationalized data as a result of unifying fragmented member information into a more usable foundation for insight, targeting, measurement, and engagement execution.
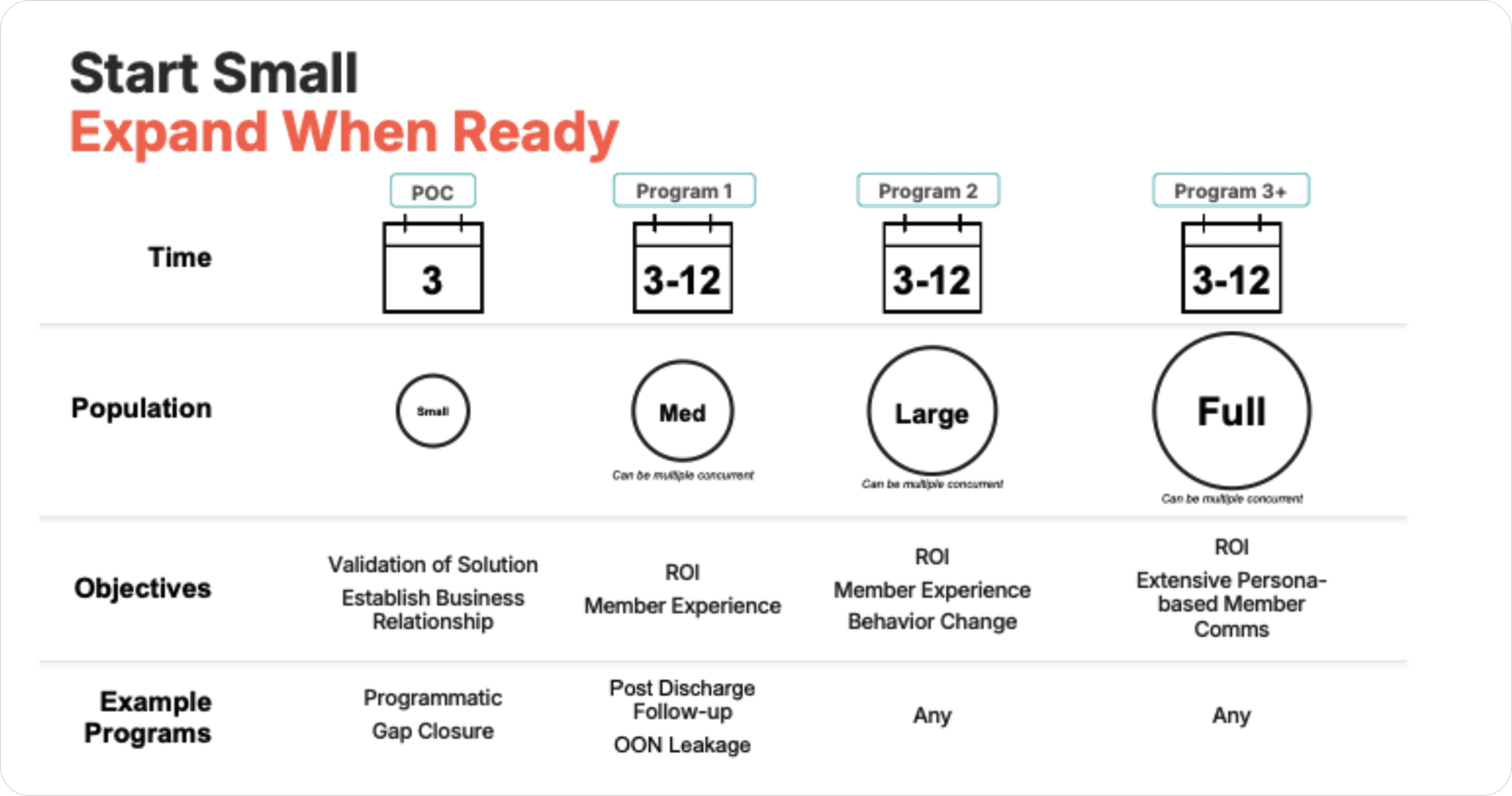
How a Customer Can Get Started with RadiantGraph
At RadiantGraph we like to follow a practical getting-started motion that is more consultative than transactional, and based on a crawl-walk-run approach. Rather than attempting enterprise-wide transformation on Day One, our approach is to start with a small population and a focused use case, validate both operational and member-experience impact, and then scale into additional programs and populations over time. This “start small, expand when ready” model mitigates implementation and business risk while building confidence across stakeholders.
The process begins with needs discovery, where the customer and RadiantGraph level-set on business priorities, current workflows, tools, roles, and target use cases. Stakeholders typically include marketing operations, data experts, and platform owners. See Appendix 1 for potential use cases based on LOB.
Discovery is followed by solution design where RadiantGraph develops an initial design for the chosen use case and shares a first-pass data checklist.
After solution review and sign-off, we share a Joint Execution Plan which details the steps involved to get us collectively to Go Live. The JEP typically includes steps for security review, an MNDA, and a BAA which start at this stage.
Once the parties confirm scope, timing, and commercial terms, we move into contracting.
Then comes kickoff, data ingestion, deploy, and Go Live. Data ingestion timing varies by customer, starting with as little as two weeks.
From a buyer’s perspective, a pragmatic path to value usually looks like this:
Pick one to three use cases, preferably with clear economics, such as gap closure, HRA completion, onboarding, or risk-adjustment visits.
Define success metrics, such as enrollment lift, reduced outreach volume, answer rate, gap closure, cost per registration, or human-hours saved.
Identify the data sources and existing engagement tools already in place.
Let RadiantGraph unify and enrich the relevant data through the Health Data Engine.
Launch the focused pilot.
Expand into additional use cases once ROI is demonstrated.
This deployment philosophy is consistent with RadiantGraph’s broader positioning: fast time to value, limited resource burden on the customer, and reinforcement of existing investments rather than forcing a large-scale replacement project.
Final Thoughts
Healthcare organizations already possess enormous amounts of data. What they often lack is a practical way to turn that data into timely, precise, and trusted engagement. This is the gap RadiantGraph closes.
The RadiantGraph approach, called Intelligent Personalization, connects four things healthcare has historically struggled to connect at the same time and in a meaningful way: data unification, decision intelligence, personalization, and compliant omnichannel execution. The result is not simply more emails with better messaging. It is a more proactive operating model for engagement, one that can help plans and healthcare organizations identify needs earlier, personalize support more effectively, reduce operational waste, and improve both business and clinical outcomes.
For organizations facing pressure to improve STARs, activate consumers, reduce cost to serve, protect limited care-team capacity, or get more value from existing engagement systems, Intelligent Personalization offers a concrete path forward. It is not a promise that more outreach will solve the problem, our thesis is that better intelligence, better timing, better prioritization, and better orchestration can. Learn more by visiting RadiantGraph.com
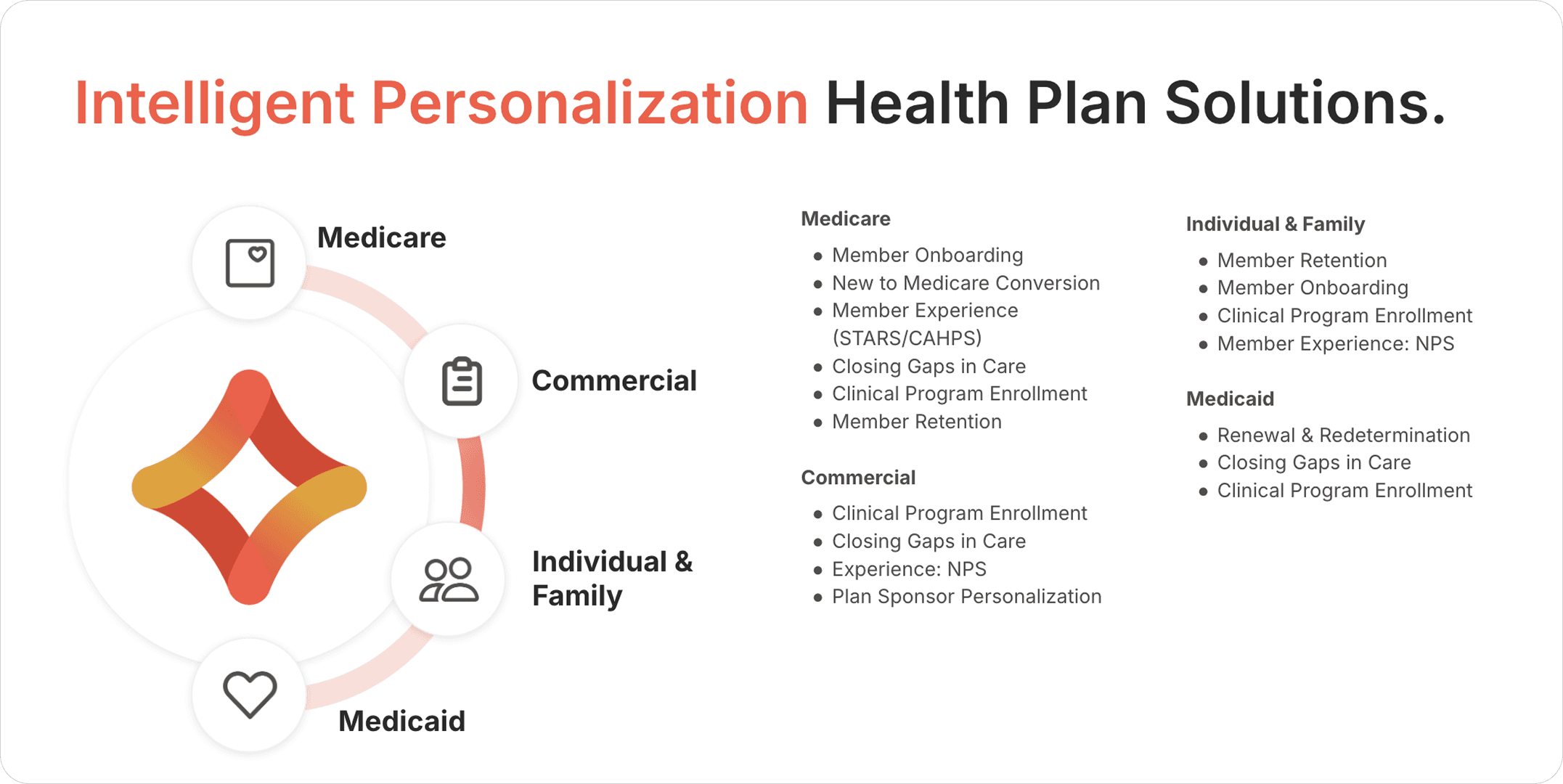
Appendix 1 – Use cases and value by Line of Business